Loss of Several tooth
People who have lost several teeth decide to try replacing them many times for purely cosmetic reasons, especially for anterior teeth.
But, in addition, there are functional reasons to replace missing teeth. Losing multiple teeth decreases chewing ability, especially if the missing teeth are back teeth (which is where most of the chewing of food occurs). If nothing is done to replace the missing teeth, there is a risk of mobilization of the teeth of the opposing arch and that the neighboring teeth will shift into the edentulous space (where teeth are missing), causing problems in the neighboring teeth that increase the chances of these being lost too.
The bone where the missing teeth were housed begins to atrophy immediately after tooth loss.
Fortunately, there are a number of options available to treat multiple missing teeth. These options include implant-supported fixed partial denture, neighboring tooth-supported fixed partial denture (“bridge”), and removable partial denture (mobile denture “hooks” attached to neighboring teeth). While some options are less expensive and more traditional, other new options may offer better long-term results.
Advantages and disadvantages of each option
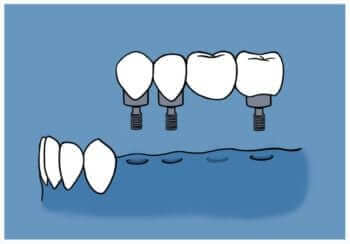
Option 1. Fixed partial prosthesis over implants.
In this treatment option, the partial prosthesis is held in place, anchored to implants that are placed in the patient’s bone, and that act as artificial roots.
Advantages
The main advantage of this procedure is that it is not necessary to carve (“wear”) the teeth next to the “hole”, thus avoiding the risks of cavities, pulp damage or irritation of the gum in the adjacent teeth, associated to conventional fixed partial dentures on teeth (“bridges”).
There is a preservation or stabilization of the bone around the implants, after they have been placed in the places that previously occupied the roots of the missing teeth.
The prosthesis can be designed so that it can be removed by the dentist for repair or updating if necessary (prostheses screwed onto implants).
Disadvantages
Occasionally, the screw that retains the prosthesis may loosen, the crown may be debased, fractures may appear in it or failure of one of the implants. However, it should be noted that clinical studies show that 90% of implants (Branemark system) placed 20 years ago for the rehabilitation of patients who had lost all their teeth are still working today. Implants used in patients with multiple missing teeth have a similar degree of success.
The prosthesis does not replace atrophied bone and soft tissue, so a bone or soft tissue graft may be necessary during implant placement. This option requires one or two surgical procedures, and a longer treatment time than conventional dentures on teeth (bridges ”).
How is implant treatment performed?
Photographs and X-rays of the patient’s mouth are taken at the initial consultation. Sometimes a special study (scan or CT) is requested, which is carried out in a radiological center outside the consultation. This study allows to see precisely (even in 3 dimensions) the quantity and quality of bone that the patient has, and helps a lot in the planning of the treatment. It may be necessary to fabricate a special provisional prosthesis (splint) that the patient wears during the radiological examination, so that the position that the dentist wishes for the artificial teeth will also appear on the scanner. The surgeon and dentist, working as a team, determine the number of implants, their position and the design of the final prosthesis.
The implants are placed in the first surgery. Before the temporary prosthesis can be replaced, the dentist must adjust the prosthesis so that it does not overload the implants during the waiting time for the implants to integrate (“weld” to the bone).
The bone must heal around the implants for a period of approximately 3 months, and then, if the implants are covered under the gum, the second surgery is performed, to verify that the implants are integrated (“welded” to the bone) . The surgeon exposes the implants in the second surgery and inserts the second component that emerges through the gingiva (called the healing abutment), and checks that the implants are immobile and without bone loss. If your surgeon has chosen a single surgical phase, he will have placed the healing abutments during the first operation, and this second intervention will not be necessary, and he will only check that the implants are integrated (“welded” to the bone), without mobility or inconvenience. After a new waiting period of 7-10 days, in which the patient must not wear the prosthesis for the gingiva to heal, the patient visits his dentist to have the temporary prosthesis adjusted again.
Subsequently, the restorative dentist begins the manufacture of the fixed prosthesis. These procedures include preliminary impression, final impression, wax-up, metal try-in, ceramic try-in, and prosthesis insertion. Once all the adjustments that satisfy both the dentist and the patient have been made, the patient begins regular maintenance and reassessment visits. The duration of implant treatment is longer than that of the other options that will be presented below (bridges over teeth and removable prostheses). However, many patients who currently wear fixed partial dentures on implants tell us that they are very comfortable with them and that the replaced teeth feel and function like their own natural teeth.
What is a bone graft?
Titanium dental implants have revolutionized the rehabilitation of patients with tooth loss. But, to be able to place the implants, it is necessary that there be a sufficient quantity and quality of bone.
Patients who do not have minimal bone conditions can also be rehabilitated by combining bone reconstruction with grafts, and the replacement of lost teeth with implants. Bone grafts obtained from the patient are the material of choice for the reconstruction of lost bone. Most of the time, reconstruction can be done by taking, under local anesthesia, a small amount of bone from another part of the mouth, and then placing it in the area where it is needed for the implant.
Bone loss varies from patient to patient, and from one area of the mouth to another. In some patients, there is a severe loss of bone and soft tissue of the gums, which compromises the final result of the treatment. In these patients, a tissue augmentation technique must be performed prior to or simultaneously with implant placement. The area where the implant will be placed is augmented with a bone graft and / or a soft tissue graft (connective graft). This is necessary to try to achieve a better cosmetic result or to give the implant a better chance of success.
Grafts are not necessary for all implants, but they are very often needed in the upper jaw (upper teeth).
If successful, augmentation techniques can make it possible to place implants in patients who would not initially be considered candidates due to lack of sufficient bone. Success rates for implants placed in reconstructed bone with bone grafts exceed 90%.
The most frequent cause of complications with bone grafts is usually the consequence of opening of the mucosa, with early exposure of the graft to the intraoral environment, bacterial contamination and loss of the graft. Patients with a smoking habit and poor oral hygiene are at higher risk for complications.
In the upper jaw, it is very common to have the gingiva thicken in the region where the implant has been placed by means of a soft tissue graft (connective tissue graft), which is taken under local anesthesia of the palate or the maxillary tailpiece region. (“wisdom tooth”). The use of connective grafts allows to achieve a better aesthetic result of the prosthesis, and helps to maintain the stable result over the years, reducing the chances of gum retractions.
The importance of maintaining hygiene
Importantly, whatever treatment is selected, success depends on a regular oral hygiene maintenance program with the dentist. All teeth need care whether they are natural or prosthetic.
If you have any questions regarding your treatment options please contact your surgeon or dentist.